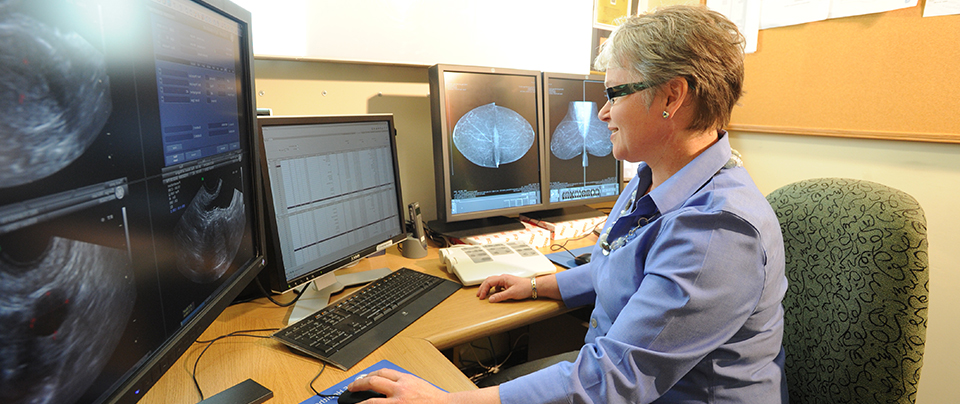
Mammography is a specific type of imaging that uses a low-dose X-ray system for examination of the breasts. Most medical experts agree that successful treatment of breast cancer often is linked to early diagnosis. Mammography plays a central part in early detection of breast cancers because it can usually show changes in the breast up to two years before a patient or physician can feel them.
Initial mammographic images themselves are not always enough to determine the existence of a benign or malignant disease with certainty. If a finding or spot seems suspicious, your radiologist may recommend further diagnostic studies.
Diagnostic mammography is used to evaluate a patient with abnormal clinical findings, such as a breast lump or lumps that have been found by the woman or her doctor. Diagnostic mammography may also be done after an abnormal screening in order to determine the cause of the area of concern on the screening exam.
Benefits
- Breast imaging improves a physician's ability to detect small tumours. When cancers are small, the woman has more treatment options, and a cure is more likely.
- The use of screening mammography increases the detection of small abnormal tissue growths confined to the milk ducts in the breast. These early tumours cannot harm patients if they are removed at this stage and mammography is the only proven method to reliably detect these tumours.
Risks
- The effective radiation dose from a mammogram is about 0.7 mSv, which is about the same as the average person receives from background radiation in the environment over three months.
- Women should always inform their doctor or X-ray technologist if there is any possibility that they are pregnant. They will be asked if they could be pregnant before their examination.
- Five to 10 per cent of screening mammogram results are abnormal and require more testing (more mammograms, fine needle aspiration, ultrasound or biopsy), and most of the follow-up tests confirm that no cancer was present. It is estimated that a woman who has yearly mammograms between ages 40 and 49 would have about a 30 per cent chance of having a false-positive mammogram at some point in that decade, and about a seven to eight per cent chance of having a breast biopsy within the 10-year period. The estimate for false-positive mammograms is about 25 per cent for women ages 50 or older. (False-positive means that the mammogram indicates there could be cause for concern, in the absence of any.)
Preparing for the procedure
Before scheduling a mammogram, it is recommended that you discuss any new findings or problems in your breasts with your doctor. In addition, inform your doctor of any prior surgeries, hormone use, and family or personal history of breast cancer. Do not schedule your mammogram for the week before your period if your breasts are usually tender during this time. The best time to schedule is one week after your period. Always inform your doctor or X-ray technologist if there is any possibility that you are pregnant.
We also recommend you:
- Do not wear deodorant, talcum powder, or lotion under your arms or on your breasts on the day of the exam. These can appear on the X-ray film as calcium spots.
- Describe any breast symptoms or problems to the technologist performing the exam.
- If possible, obtain prior mammograms and make them available to the radiologist at the time of the current exam.
- Ask when your results will be available; do not assume the results are normal if you do not hear from your doctor or the mammography facility.
In addition, before the examination, you will be asked to remove all jewellery and clothing above the waist and you will be given a gown or loose-fitting material that opens in the front.